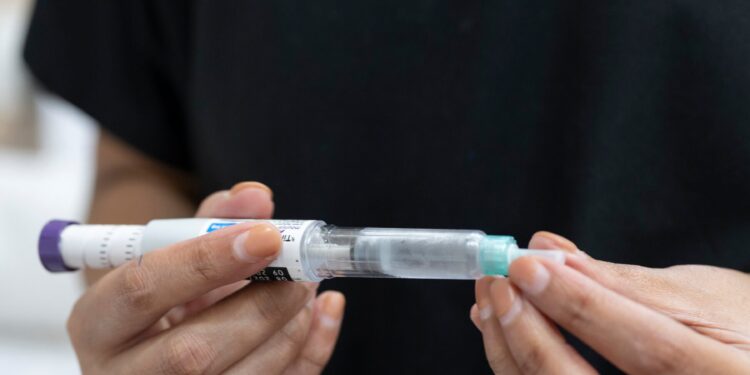
Generic Ozempic Could Cut Prices for 40% of the World’s Population
- Patent expiry in India, China, Canada, Brazil, Turkey and South Africa slated for this weekend.
- More than 800 million adults in India and China are obese or overweight.
- Over 360 million adults in the same markets live with diabetes.
- U.S. and European generic entry not expected until the early 2030s.
Why a generics wave matters for global health equity
OZEMPIC—The blockbuster GLP‑1 drugs sold as Ozempic and Wegovy are about to lose their monopoly in nations that together house roughly 40 percent of humanity.
On Saturday, Novo Nordisk will lose patent protection in several of the world’s most populous countries, paving the way for generic manufacturers to launch versions as early as this weekend in India.
Activist Leena Menghaney says the shift will “democratize” a treatment that has been restricted to the wealthy, potentially transforming the lives of hundreds of millions of patients.
The Scale of Obesity and Diabetes in India and China
India and China together account for more than 800 million adults who are classified as obese or overweight, according to the World Obesity Atlas 2025. That figure represents roughly one‑third of the global adult population facing weight‑related health risks.
Diabetes adds another layer of urgency
In addition to the weight‑related burden, the Lancet’s 2024 diabetes analysis estimates that over 360 million adults in these two nations live with diabetes, a condition that GLP‑1 agonists like Ozempic can help manage and even reverse.
These numbers illustrate why the arrival of generic Ozempic could be a public‑health watershed. The drug’s dual efficacy—promoting weight loss while improving glycemic control—means that a price‑accessible version could simultaneously address two of the most pressing chronic disease challenges in the region.
Health economist Dr. Ananya Rao of the Indian Institute of Public Health notes that “the convergence of obesity and diabetes in South Asia creates a perfect storm for demand. Generic entry will likely expand treatment coverage from a privileged few to millions of patients who currently cannot afford brand‑name therapy.”
Beyond individual health, broader economic implications loom. The World Bank estimates that untreated diabetes costs low‑ and middle‑income economies up to 2 percent of GDP annually. Lowering drug prices could therefore translate into macro‑level fiscal benefits.
While the numbers are staggering, they also provide a concrete metric for policymakers to gauge the impact of generics on health outcomes.
As the generic wave approaches, the next question is how quickly supply chains can meet this massive demand.
Understanding the timeline of patent expiry and market entry will set the stage for assessing price dynamics.
When Will Patents Expire? – A Timeline of Generic Entry
Patent protection for Novo Nordisk’s semaglutide molecules is set to lapse in a staggered fashion across key markets, triggering the first wave of generics.
Key dates mapped out
Saturday marks the official loss of patent rights in India, opening the door for local manufacturers to file for approval. Within days, generic versions are expected to appear on Indian pharmacy shelves.
In the months that follow, China, Canada, Brazil, Turkey and South Africa are slated to see their own generic launches, though exact dates vary by national regulatory timelines.
Regulatory analyst Maya Liu of the Shanghai Institute for Pharmaceutical Policy explains, “China’s fast‑track approval pathway for generics means we could see market entry within three to six months after the patent expiry announcement.”
Conversely, the United States and European Union have enacted “patent term extensions” and “data exclusivity” provisions that push generic competition back to the early 2030s, a strategic move intended to preserve incentives for drug innovation.
The divergent timelines highlight how intellectual‑property law shapes global health access, creating a patchwork of availability that mirrors economic power.
Stakeholders—from ministries of health to patient advocacy groups—must therefore navigate a complex calendar to coordinate procurement, insurance coverage, and public‑health messaging.
With the timeline clarified, the next chapter examines how price dynamics are likely to shift once generics hit the market.
Price Shock: What Generic Ozempic Could Mean for Patients
When a blockbuster drug loses its patent, price reductions of 60‑80 percent are common, according to data from the Indian Ministry of Health on previous generic launches. While exact figures for Ozempic remain to be published, analysts project a similar trajectory.
Projected cost savings for patients
Current brand‑name Ozempic prices in India hover around ₹12,000 (≈ $150) per month, a cost unaffordable for most of the country’s 1.4 billion residents. A 70 percent price cut would bring the monthly cost down to roughly ₹3,600, expanding eligibility for government‑subsidized programs.
Health policy expert Dr. Ramesh Patel of the All‑India Institute of Medical Sciences notes, “Such a reduction could increase uptake by an order of magnitude, moving the drug from a niche therapy to a mainstream public‑health tool.”
Beyond individual savings, the aggregate economic impact is striking. If even 5 percent of the 800 million obese adults in India and China begin treatment, the annual drug‑spending burden could fall by up to $10 billion globally.
Insurance providers in Canada anticipate similar dynamics. A generic entry could lower the average reimbursement rate from CAD $150 to roughly CAD $45 per dose, easing pressure on provincial health budgets.
These price dynamics also reverberate through the pharmaceutical supply chain, prompting brand‑name manufacturers to explore new revenue streams such as combination therapies or next‑generation formulations.
With price expectations clarified, the next chapter explores why the United States and Europe will not see comparable savings for another decade.
Regulatory Protections: Why the West Waits Until the 2030s
In the United States and the European Union, Ozempic will not become generic until the early 2030s, a delay rooted in policy mechanisms designed to spur pharmaceutical innovation.
Data exclusivity and patent term extensions
Both jurisdictions grant brand‑name drugs up to ten years of data exclusivity, meaning competitors cannot rely on the original clinical trial data for approval. Additionally, the U.S. Hatch‑Waxman Act allows for up to five years of patent term extensions to compensate for regulatory delays.
Legal scholar Prof. Elena García of Harvard Law School explains, “These extensions are a double‑edged sword: they protect R&D investments but can also lock out affordable alternatives for years, especially for high‑cost biologics.”
Pharmaceutical industry analysts estimate that the combined effect of exclusivity and extensions adds roughly a decade of market protection for drugs like Ozempic, compared with the 5‑year window seen in many low‑ and middle‑income markets.
Patient advocacy groups in the U.S., such as the Diabetes Coalition, argue that “the public health cost of delayed generic entry outweighs the marginal innovation incentives for a drug that already has multiple approved indications.”
Meanwhile, Novo Nordisk has signaled plans to launch a next‑generation semaglutide formulation in the West, potentially extending its premium pricing strategy beyond the current patent horizon.
The regulatory divergence underscores a broader tension between incentivizing drug development and ensuring equitable access—a balance that will shape future policy debates.
Having examined the policy backdrop, the final chapter asks whether broader access will translate into measurable health improvements.
Will Wider Access Translate Into Better Health Outcomes?
Access alone does not guarantee improved health metrics; the real test lies in whether patients can adhere to therapy and whether health systems can integrate the drug into standard care pathways.
Evidence from past generic roll‑outs
When generic antihypertensives entered the Indian market in 2015, hypertension control rates rose from 12 percent to 28 percent within three years, according to a study by the Indian Council of Medical Research.
Applying that precedent, public‑health researchers at the University of Toronto project that a 70 percent price cut for Ozempic could increase treatment uptake among eligible diabetics from 5 percent to 20 percent within five years, potentially averting an estimated 150,000 cardiovascular events.
Dr. Priya Singh, an endocrinologist at Delhi’s All‑India Institute of Medical Sciences, cautions, “Affordability is necessary but not sufficient. We need robust patient education, supply‑chain reliability, and insurance coverage to realize the drug’s full potential.”
In Canada, provincial health ministries are already drafting reimbursement frameworks that tie coverage to demonstrated weight‑loss outcomes, a model that could be exported to other markets.
Ultimately, the generics wave presents a natural experiment: researchers will be able to compare health outcomes across countries with staggered generic entry, shedding light on the causal impact of drug affordability.
If the anticipated surge in usage materializes, the global burden of obesity‑related disease could see a measurable decline, marking one of the most significant public‑health victories of the decade.
Thus, the arrival of generic Ozempic is more than a market event; it is a test of whether price reductions can catalyze systemic health improvements worldwide.
Frequently Asked Questions
Q: When will Ozempic become generic in India?
Novo Nordisk loses patent protection on Saturday and generic versions are expected to hit Indian pharmacies as early as the following weekend.
Q: Why won’t Ozempic go generic in the U.S. and Europe until the 2030s?
Special regulatory extensions in the United States and Europe protect brand‑name drugs to encourage innovation, delaying generic entry until the early 2030s.
Q: How many people could benefit from generic Ozempic in India and China?
Together, India and China have more than 800 million adults who are obese or overweight and over 360 million adults living with diabetes, representing a massive potential patient pool.